Hormone Treatment
The purpose of the hormone treatment is to stimulate the ovaries to produce more than the one follicle that a woman produces in a normal cycle. The hormone stimulation aims at making 8-12 eggs for oocyte pick-up, but in some instances less will do. The number of cells can vary a lot depending on the woman’s age and response to the stimulation.
We monitor the follicle growth by transvaginal ultrasound scans. In this way, the size and number of follicles can be determined. The size of the follicle indicates the maturity of the egg contained in the follicle. When the follicles have reached a size of 17-20 mm the eggs are mature and ready for oocyte pick-up. The oocyte itself has a diameter of 0.12 mm and is not visible at the ultrasound scan.
In our clinic, we use different hormone stimulation schemes. We mostly use treatment with ‘long down- regulation’ (we call it scheme 3) and the so-called ‘short antagonist protocol’ (we call it scheme 4). In some cases we use stimulation based on chlomiphene citrate, ‘agonist flare-up’ or ‘CRASH’. Very rarely, we may do IVF without hormone stimulation.
The treatment is always tailored to the individual woman based on her cause of infertility and on experience from previous successful or less successful treatments.
When a treatment cycle starts, we will provide you with detailed information about the treatment plan, use of medicine, possible side effects and we plan the next consultation and ultrasound scan.
- Scheme 0: No hormone stimulation
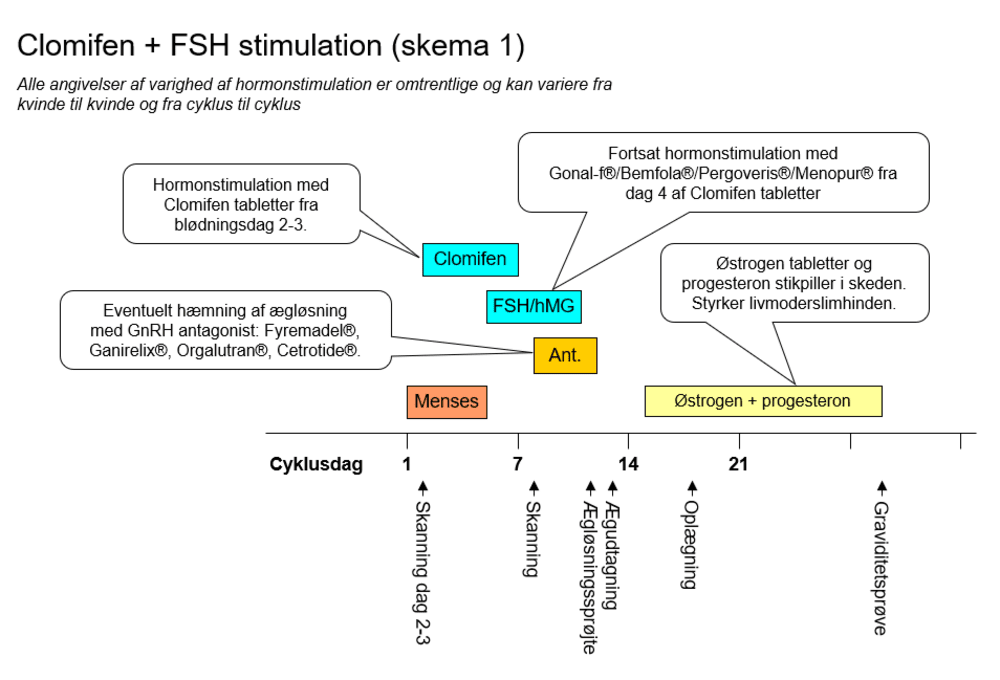
- Scheme 1: Stimulation with Pergotime® tablets possibly combined with hormone injections
- Scheme 2: Short agonist protocol
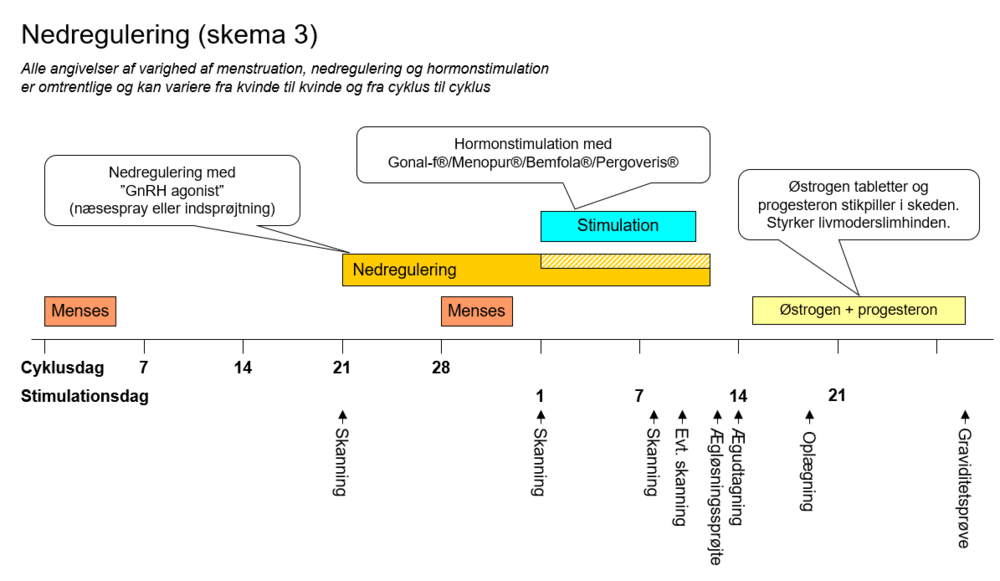
- Scheme 3: Long down-regulation
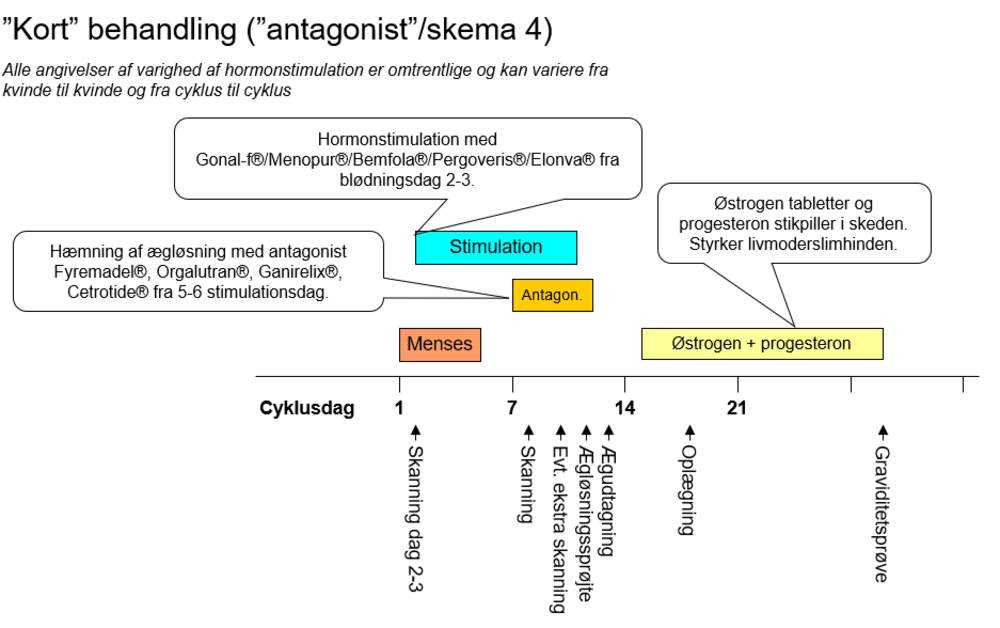
- Scheme 4: Short antagonist-protocol
Click on schedules for larger viewing. Schedules 0 and 2 are not shown.
Scheme 3: Long down-regulation
Scheme 4: Short antagonist-protocol
Scheme 1: Stimulation with Pergotime®